 In addition, CT and MRI are useful as combined diagnostic imaging methods (11). Large ventricular septal defect is nearly always present (10).įigure 8: Postoperative chest CT angiogram 3D reconstruction.Īlthough echocardiography has some limitations in evaluating the aortic arch and the descending aorta, it is the technique of choice for detecting concomitant cardiac abnormalities. Blood flow to the descending aorta depends on the patency of the ductus arteriosus and, because it is almost always widely patent at birth, a collateral circulation does not develop and death occurs when the ductus closes soon after birth. If the IAA is left untreated, 90% of the affected infants die at a median age of 4 days (9). 4).įigure 7: Circumflex artery Y venous graft anastomosis to the LIMA.Ītresia of the aortic arch should be differentiated from IAA, as the latter is characterized by a complete lack of anatomic continuity between the transverse aortic arch or isthmus and the descending thoracic aorta (1-5). The pericardium was opened in a longitudinal fashion, exposing the descending thoracic aorta (Fig. Care was taken not to injure the esophagus on the right by palpation of a nasogastric tube previously positioned into the esophagus. Distal saphenous anastomoses of the circumflex artery and right coronary artery were made, and the cardiac apex was then elevated out of the pericardial sac to expose the posterior pericardium (Fig. Cardiopulmonary bypass (CPB) was then initiated under moderate hypothermia. The aorta was cross-clamped, and antegrade Del Nido cardioplegia was delivered through the aortic root to induce diastolic cardiac arrest. Flow was adequate, although the LIMA was found to have significant atherosclerosis. The left internal mammary artery (LIMA) was dissected in a skeletonized fashion. Differential blood pressure was closely monitored during surgery, with radial and femoral arterial lines to confirm accurate distal perfusion. Arterial cannulation was on the ascending aorta and the venous cannula was inserted into the right atrial appendage for venous return. Atresia of the aortic arch is observed.Ī single-stage operation was performed through a midline sternotomy. Cerebral magnetic resonance imaging (MRI) demonstrated diffuse lacunar infarcts with no evidence of berry aneurysms in the circle of Willis.įigure 2: Chest angiography CT. The descending thoracic aorta was dilated distal to the occlusion zone and it was supplied by prominent collateral circulation from internal mammary arteries, intercostal arteries, and the vertebrobasilar system (Fig. Aortic occlusion is evident.Ĭhest computed tomography (CT) angiography revealed atresia of the aortic arch distal to the origin of the left subclavian artery. Radial access cardiac catheterization showed significant proximal stenosis of the left anterior descending artery, circumflex artery, and right coronary artery.įigure 1A and 1B: Thoracic aortogram. Echocardiography revealed segmental contractility disorders, bicuspid aortic valve with neither stenosis nor regurgitation, normal diameter of the ascending aorta, and aortic coarctation distal to the origin of the left subclavian artery.įemoral access cardiac catheterization showed complete occlusion of the thoracic descendent aorta distal to the left subclavian artery, without passage of the wire through the occlusion zone and with an 85 mm Hg gradient (Fig. The blood pressure was 173/102 mm Hg in the left arm, 174/101 mm Hg in the right arm, and 66/51 mm Hg in the right leg. On physical examination, peripheral pulses were palpable over the carotid arteries and in the upper limbs, but inguinal pulses were almost imperceptible. These symptoms had begun several months earlier and were accompanied by recent angina pectoris. In 2017, a 45-year-old man presented at the authors’ hospital because of dyspnea on exertion, swelling of his legs, and orthopnea. In this case report, the authors describe the history of a 45-year-old man with symptomatic heart failure secondary to atresia of the aortic arch and associated coronary artery disease. In atresia of the aortic arch, continuity between the segments is achieved by an imperforate, fibrous cord of variable length, although the hemodynamic and physiological effects may be identical in both entities (1-3). 
It must be anatomically differentiated from an interrupted aortic arch (IAA), which is characterized by a complete lack of anatomic continuity between the transverse aortic arch or isthmus and the descending thoracic aorta (1-5). 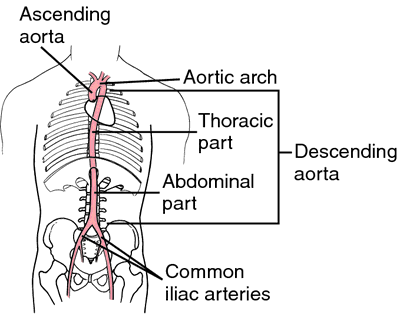
Atresia of the aortic arch is a rare condition among adults. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
